NYU Professor Fired for Giving Students Bad Grades

GUEST POST from Arlen Meyers, M.D.
A recent article described the termination of an NYU organic chemistry professor in response to a student petition. When the professor pushed students’ grades down, noting the egregious misconduct, he said they protested that “they were not given grades that would allow them to get into medical school.” The reporter noted that, in short, this one unhappy chemistry class could be a case study of the pressures on higher education as it tries to handle its Gen-Z student body. Should universities ease pressure on students, many of whom are still coping with the pandemic’s effects on their mental health and schooling? How should universities respond to the increasing number of complaints by students against professors? Do students have too much power over contract faculty members, who do not have the protections of tenure?
And how hard should organic chemistry be anyway? One faculty member said, “Unless you appreciate these transformations at the molecular level, I don’t think you can be a good physician, and I don’t want you treating patients.”
I know the feeling. While organic chemistry is termed a “doctor killer” by premedical students, getting any grade less than an “A”, typically in science, technology, engineering, or math subjects, can doom your application. When I saw that B I got in physics in my junior year of college, I started thinking about Plan B. Then I really learned the gravity of the situation.
Despite the noise and groaning, medical school applications continue to rise, driven by many factors. However, the medical school education model dates back to the Flexner report issued in 1910. Many are trying to address the challenges of how to train the biomedical research and practice workforce to win the 4th industrial revolution, but progress has been slow. Here were the challenges facing medical schools in 2015. Things have not radically changed. Medical educators, particularly those in public medical schools, will continue to face several basic problems in the coming years. The “invisible enemy” has exacerbated many.
We should rethink how we recruit and accept medical students.
Here are some questions that should inform that transition:
1. Do doctors really need to be that “smart”? GPAs can vary significantly across different medical schools, so it pays to do your research before applying. The Association of American Medical Colleges (AAMC) reported an average GPA for medical school of 3.60 across all applicants for the 2021-2022 application cycle. For the same year, applicants had an average science GPA of 3.49 and an average non-science GPA of 3.74.
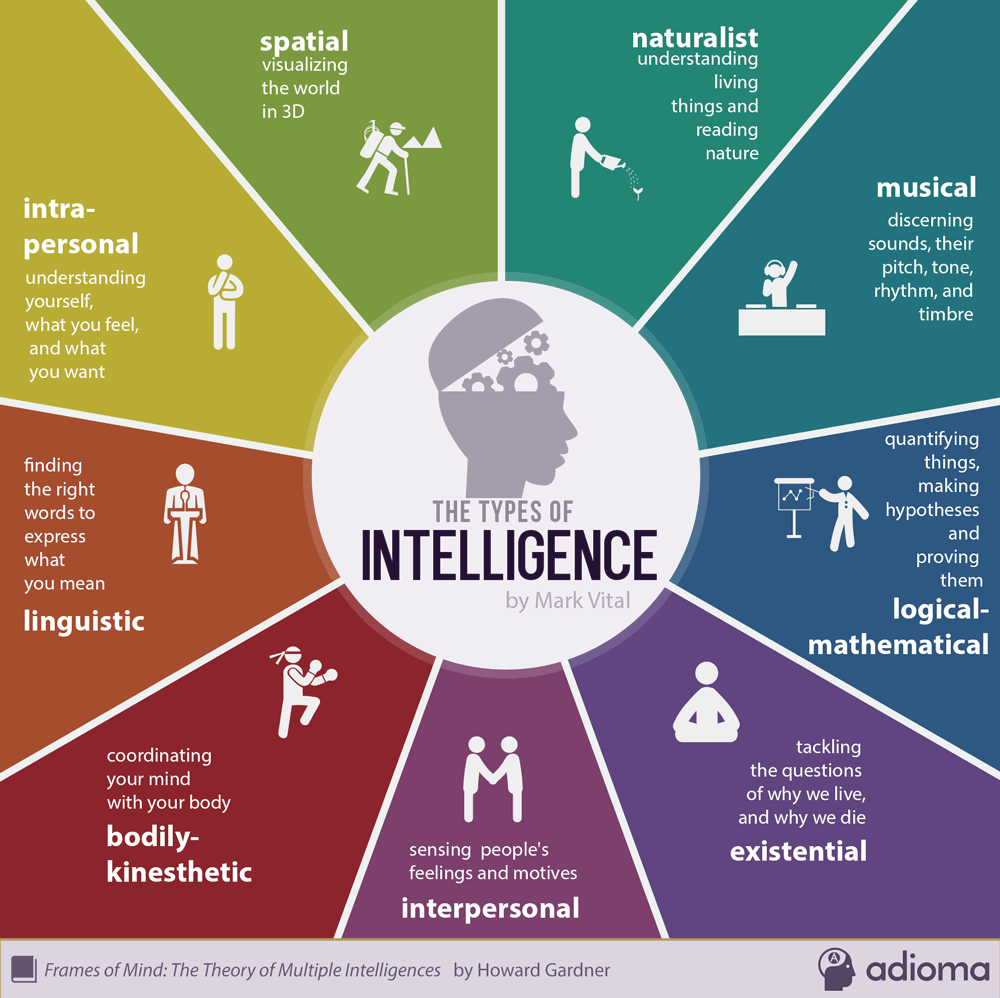
2. What kind of intelligence do doctors need to meet the needs of their stakeholders and communities?
3. Do patients really care what grade their doctor got in organic chemistry, or, for that matter, whether they graduated last in their class from medical school?
4. How has the pandemic and the persona of Gen Z changed medical education?
5. What do doctors and patients need to know to win the 4th industrial revolution? Organic chemistry?
6. How does the present system and its reliance on undergraduate STEM academic performance impact inequitable socioeconomic and demographic acceptance rates?
7. How should we transform premedical, medical, and post-graduate pedagogy? Examples are project-based learning and peer reviewed feedback.
8. Why do we insist that undergraduates declare a major?
9. Is the purpose of a medical school education solely to graduate students who have the knowledge, skills, abilities, and competencies to take care of patients, or should we provide them with exit ramps too?
10. How do we balance a medical culture of conformity with a culture of creativity?
11. What will be the future of medical work?
I’m lucky that I dodged the bullet. But I still have Plan B.
Image Credits: Adioma (Mark Vital), Pixabay
![]() Sign up here to get Human-Centered Change & Innovation Weekly delivered to your inbox every week.
Sign up here to get Human-Centered Change & Innovation Weekly delivered to your inbox every week.
